If your parrot or cockatoo is losing feathers, growing in twisted or damaged ones, or showing beak changes you can't explain, PBFD (psittacine beak and feather disease) is one of the first things that should be on your radar. It's one of the most serious viral diseases affecting parrots and other psittacine birds, and the symptoms can be easy to confuse with molting problems, nutritional deficiencies, ...or even parasites. The tricky part is that visual signs alone are never enough to confirm it. Here's what to look for, how to make sense of what you're seeing, and exactly what to do today.
PBFD bird symptoms: signs, diagnosis, and next steps

Quick PBFD Overview: What It Is and Why Symptoms Matter
PBFD is caused by beak and feather disease virus (BFDV), a circovirus that attacks the feather follicles and suppresses the immune system. It affects most psittacine species, including African greys, cockatoos, eclectus parrots, lovebirds, and macaws, though how severely and how quickly it progresses varies quite a bit by species and age. Cockatiels, for example, show a different and less well-documented clinical picture than cockatoos or African greys.
The virus spreads easily through feather dust, feces, crop secretions, and contaminated surfaces. One of the most important things to understand is that an infected bird can be shedding virus into the environment before any visible symptoms appear. That's what makes early recognition so important, and why you can't wait for obvious feather changes before acting. That's what makes early recognition so important, and why you can't wait for obvious feather changes before acting. flying bird hand symptoms
The reason symptoms matter isn't just for your bird's sake. Recognizing PBFD signs early lets you isolate the bird before it exposes others, get diagnostic testing started, and begin supportive care that can genuinely improve quality and length of life, even when a cure isn't possible.
Key PBFD Bird Symptoms: Feathers, Beak, Skin, Nails, and Behavior
The most recognizable signs of PBFD involve feathers, but the full picture is broader than that. Here's what to look at across different parts of the bird.
Feather Changes

Feather abnormalities are the hallmark of chronic PBFD. Look for feathers that come in twisted, curled, stunted, or with the shaft pinched or constricted. Feathers may look frayed, have the barbs missing so they appear almost bare, or break off easily. In powder-down species like cockatoos and African greys, a noticeable reduction in that powdery sheen can be an early clue. Crucially, the pattern tends to be symmetrical, meaning both wings are affected similarly, and it becomes more obvious after each molt because dystrophic feathers progressively replace the normal ones over time.
Feather loss alone doesn't mean PBFD. The key red flag is feathers that grow in abnormally, not just feathers that fall out during a normal molt. If new feathers look wrong from the moment they emerge, that's significant.
Beak Changes
Beak involvement is a serious sign. PBFD can cause the beak to become overgrown, misshapen, or brittle. You might see the upper or lower beak deviating, cracking, or developing a necrotic (dead, darkened) appearance. The beak may also develop a dull, abnormal texture rather than the normal smooth sheen. These changes tend to develop later in the disease course but are strong visual indicators when they appear.
Skin and Nail Changes

Skin lesions are less commonly discussed but can occur, particularly in cockatiels where skin changes may be one of the more prominent signs. Nails can become overgrown or malformed in a similar way to the beak, reflecting the virus's attack on keratin-producing tissue throughout the body.
Behavioral and Systemic Signs
Because PBFD is immunosuppressive, many of the behavioral signs you'll notice are actually caused by secondary infections rather than the virus itself. Watch for lethargy, depression, loss of appetite, weight loss, and general weakness. Birds with compromised immune systems are prone to secondary bacterial, fungal, and viral infections, which can cause pneumonia, enteritis (gut inflammation), and other systemic problems. Diarrhea and crop issues are also reported, especially in younger birds.
Acute vs Subacute vs Chronic PBFD: What Signs Look Like at Different Stages

PBFD doesn't always look the same, and the form it takes depends heavily on the age of the bird and, to some extent, the species. Understanding the three main presentations will help you figure out what you might be dealing with.
| Form | Who It Affects | Key Signs | Feather Changes? |
|---|---|---|---|
| Peracute/Acute | Nestlings, very young birds; African greys | Sudden severe illness, weight loss, diarrhea, crop problems, severe blood abnormalities (low white cells, anemia), liver involvement | Often absent early on |
| Subacute | Juveniles/young adults | Systemic illness plus early feather dystrophy as first feathers emerge or next molt begins | Beginning to appear |
| Chronic | Older juveniles and adults | Progressive symmetrical feather dystrophy worsening with each molt, beak deformities, secondary infections over time | The dominant feature |
The peracute form, most notably described in African grey parrots, is particularly deceptive because it can kill quickly with very non-specific signs and no feather changes at all. If a young bird suddenly becomes severely ill with no clear cause, PBFD should be considered even without the classic feather picture.
The chronic form is the most common presentation overall. It's typically insidious, meaning it creeps up gradually. The bird looks increasingly ragged after each molt, and owners sometimes assume it's a molting problem or a nutritional issue for months before PBFD is suspected.
How to Tell PBFD Apart from Other Feather and Respiratory Conditions
This is one of the most important things to get right, because PBFD is far from the only reason a bird can have feather or beak problems. The conditions most likely to be confused with PBFD include:
- Nutritional deficiencies (particularly vitamin A deficiency), which can cause feather quality problems and beak abnormalities but tend to improve with dietary correction
- French molt (caused by avian polyomavirus), which primarily affects budgerigars and causes feather loss, especially flight and tail feathers, in young birds
- Feather-destructive behavior (plucking or chewing), where the bird removes its own feathers, typically leaving the head intact since it can't reach there itself
- External parasites such as mites or lice, which can cause feather damage and irritation (you may see the parasites or their droppings on close inspection)
- Bacterial or fungal feather follicle infections, which can cause localized feather abnormalities
- Normal heavy molts or stress molts, which can look alarming but resolve naturally
The symmetrical pattern of feather dystrophy in PBFD is a helpful distinguishing feature, as is the fact that damaged feathers don't improve with diet changes or parasite treatment. But honestly, visual differentiation is unreliable. A bird losing feathers from plucking won't have damaged feather structure in the same way, and nutritional feather problems usually affect feather quality more broadly rather than producing the specific dystrophic shapes PBFD causes. Still, none of these features are definitive on their own. That's exactly why testing is non-negotiable.
Respiratory symptoms you might notice, like labored breathing, wheezing, or nasal discharge, aren't caused directly by PBFD itself. They're usually signs of a secondary infection in an immunocompromised bird. If you're also dealing with respiratory signs alongside feather changes, the bird needs urgent veterinary attention.
What to Do Today: Isolate, Monitor, and Document Warning Signs
If PBFD is on your radar, the most important thing you can do right now is act as if the bird is contagious until proven otherwise. Here's a practical step-by-step for today:
- Isolate the bird immediately. Move it to a separate room with its own cage, food dishes, water bowls, perches, and toys. Nothing from this bird's setup should be shared with other birds in your home or aviary.
- Wash your hands thoroughly before and after handling the isolated bird and before interacting with any other birds. Change clothing if you've been in close contact.
- Do not allow any outside birds to visit your home, and do not take your birds to common bird areas like pet stores or bird clubs until you have a diagnosis.
- Document what you're seeing. Take clear photos or short video clips of the feather abnormalities, beak changes, droppings, and the bird's posture or behavior. Note when you first observed each sign and any recent events (new birds in the home, stress, illness).
- Check the bird's weight if you have a small scale. Weight loss in parrots can be subtle and is easiest to track with weekly or daily measurements.
- Call an avian vet today. Describe the symptoms, provide your photos, and ask about getting a PCR test scheduled. Many avian vets can advise on sample collection and urgency over the phone.
If the bird is showing acute signs (sudden severe weakness, not eating, difficulty breathing, collapse), treat this as an emergency and contact an avian vet or emergency animal hospital immediately. Don't wait to document things first.
How Vets Confirm PBFD: Testing and What to Expect
Clinical signs can point strongly toward PBFD, but they cannot confirm it. This is a hard rule, not a suggestion. Some birds test positive via PCR but show no feather changes at all. Others have feather dystrophy from entirely different causes. Only laboratory testing can tell you what you're actually dealing with.
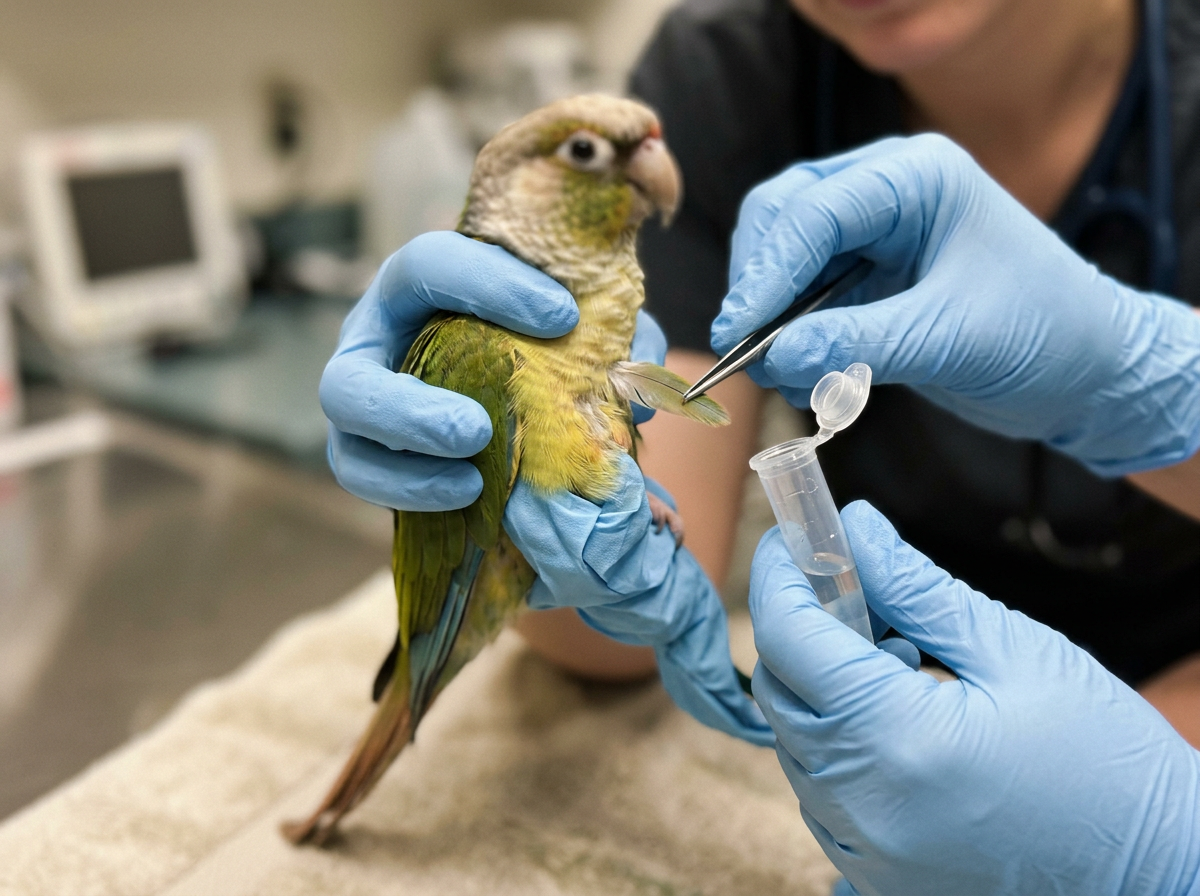
The primary diagnostic tool is PCR (polymerase chain reaction) testing, which detects the DNA of beak and feather disease virus. Samples that can be used for PCR include feather pulp (from freshly pulled feathers), whole blood, and in some protocols, environmental swabs. Blood-based PCR and feather pulp PCR are the most commonly used. If clinical signs are present but PCR results are negative or ambiguous, your vet may recommend a biopsy of affected feather follicles or skin for histopathology, which examines tissue changes under a microscope.
One important nuance: the virus sheds so heavily into the environment through feather dust and feces that environmental contamination can complicate test interpretation. This is one reason a blood sample is often preferred for a clean result. If your bird has had any contact with other PBFD-positive birds or a contaminated environment, your vet may recommend retesting roughly 45 to 60 days after the initial negative result to confirm true negative status.
When you go to the vet, bring your photos and notes. Be ready to describe when symptoms started, whether you've added any new birds recently, and whether the bird has had any contact with outside birds. This history genuinely helps the vet prioritize which tests to run and how urgently.
Treatment, Supportive Care, and Realistic Outcomes
There is currently no antiviral treatment that eliminates PBFD virus from an infected bird. That's the hard truth. But that doesn't mean there's nothing to do. Supportive care can meaningfully extend life and improve quality of life, particularly for birds in the chronic form of the disease.
Because PBFD suppresses the immune system, managing secondary infections is the cornerstone of treatment. That means antibiotics for bacterial infections, antifungals when needed, anti-parasitic treatment if parasites are present, and nutritional support to keep the bird in the best possible condition. Birds that are well-nourished and kept in low-stress environments with prompt treatment of secondary infections can live for years with PBFD, even if the feather changes don't reverse.
Outcomes are variable and depend on the form of disease, the species, and the age at diagnosis. Young birds with the peracute or acute form have a poor prognosis and can deteriorate very rapidly. Birds with chronic PBFD that are otherwise well-managed may maintain a reasonable quality of life for a considerable time. Some birds with very early or mild infection, particularly adults, may even clear the virus, though this is not guaranteed and bears monitoring with repeat testing.
Be honest with your vet about your capacity to manage a chronically ill bird. The conversation about long-term care, quality of life, and when palliative care becomes the kindest option is worth having early rather than in a crisis.
Prevention and Reducing Spread in Households and Aviaries
Whether you have one bird or an aviary full of them, the principles for preventing PBFD spread are the same. Quarantine is the single most effective measure you can implement.
Any new bird entering your home or aviary should be quarantined for a minimum of 30 days, ideally longer. During quarantine, the bird must have completely separate equipment: its own cage, perches, food and water dishes, toys, and cleaning tools. Nothing from the quarantine area should come into contact with your existing birds.
All new birds should be PCR-tested for PBFD during quarantine, even if they look healthy. Remember, infected birds can shed virus before symptoms appear. A negative test at the start of quarantine followed by a clean bill of health from an avian vet is the standard to aim for before introducing a new bird to your flock.
If you have a bird suspected or confirmed positive for PBFD, strict containment applies. According to veterinary guidance, you should have no contact with outside birds and should not bring your birds to environments where other birds are present. Items that cannot be adequately disinfected (certain porous materials, wooden perches, rope toys) should be discarded rather than cleaned and reused.
For disinfection, clean all surfaces and equipment thoroughly with soap and water first, then apply an appropriate avian-safe disinfectant. Cages, metal perches, food and water bowls, and transport carriers can all be effectively disinfected this way. The virus is hardy in the environment, so routine cleaning is not sufficient when PBFD is in play.
If you're in a rescue or breeding environment, the stakes are higher. All birds coming in should be screened, all positive birds should be isolated from negative ones indefinitely, and separate equipment and staff protocols should be maintained for each group. Feather dust is the major environmental contaminant, so ventilation and air filtration matter too.
While you're waiting for test results, maintain the isolation protocol as if the result will be positive. The time between suspicion and confirmation is when transmission risk is often highest, especially because many birds are already shedding virus before the clinical picture is obvious. Staying cautious during that window is one of the most protective things you can do for the rest of your birds.
FAQ
Can pbfd bird symptoms be mistaken for a “normal” molt, and how can I tell if I should treat it as more than molting?
Yes. The key difference is whether feathers look wrong as they emerge (twisted, pinched shafts, frayed new feathers), not just that older feathers shed. If you see a symmetrical pattern on both sides and the new feathers stay abnormal through multiple molts, treat it as suspicious and contact an avian vet for PCR testing rather than waiting.
My bird has feather dust and some feather loss, but no obvious beak changes. Can it still be PBFD?
PBFD can present without beak abnormalities, especially early or in some species, and infected birds can shed virus before visible changes. If feather structure looks dystrophic or powder sheen steadily declines, assume risk and get a test, even if the beak seems normal.
If PCR testing is negative once, do I have to worry about a false negative?
Sometimes. Because contamination from feather dust can complicate interpretation, a blood-based PCR is often preferred for clarity. If the bird had known exposure to a contaminated environment or other birds, your vet may recommend repeat testing around 45 to 60 days to confirm a true negative.
What sample should I request for pbfd bird symptoms testing, feather pulp or blood?
Ask your avian vet what sample type best matches your situation. In many cases, blood-based PCR can reduce the chance of environmental contamination affecting results. Feather pulp PCR can still be appropriate, but your vet may choose based on how severe the lesions are and what sampling is safest and most practical for your bird.
Should I start vitamins or a parasite treatment before I know if it’s PBFD?
Avoid “trial-and-error” management as a substitute for diagnosis. Diet changes can be supportive, but they will not correct the specific feather-shaft dystrophy patterns typical of PBFD, and delaying testing increases spread risk. If parasites are present, they should be treated once a vet advises, while you proceed with PCR and isolation.
What are early behavioral signs that pbfd bird symptoms might be starting, even if the feathers look mostly okay?
Look for subtle immune-related decline such as reduced appetite, quieter behavior, weight loss, or lethargy that seems out of proportion to normal seasonal changes. Respiratory signs like wheezing or nasal discharge usually point to secondary infections, which still require urgent avian evaluation.
How fast can PBFD progress in the peracute form, and is “no feather changes” ever okay to ignore?
In some young birds, especially in peracute presentations, deterioration can be rapid and feather changes may be absent. If a young bird becomes suddenly very ill without an obvious cause, PBFD should be part of the urgent differential, and emergency veterinary care should not be delayed.
What precautions should I take at home while waiting for PBFD test results?
Act as if the bird is contagious. Isolate it, use separate cage cleaning tools, and avoid letting feather dust circulate (limit moving bedding around, cover/contain waste during cleaning). Do not allow contact with other birds or outside birds’ areas, and transport only if your vet instructs it as an emergency.
Can I disinfect wood perches, rope toys, or other porous items if I suspect PBFD?
If the item cannot be disinfected thoroughly, it should be discarded rather than cleaned and reused. Porous materials and items that trap feather dust are hard to reliably decontaminate, so replacing them is safer than assuming disinfection will eliminate virus.
If my other birds have been exposed, do they all need PCR testing immediately?
At minimum, discuss testing with your avian vet. The usual approach is to quarantine the exposed birds and test them even if they look healthy, because shedding can occur before symptoms. A negative result at the start may be followed by retesting if there was significant exposure or if the initial sample could be affected.
What does supportive care for PBFD involve day to day, especially regarding secondary infections?
Expect a medical focus on preventing and treating secondary problems, since immunosuppression is central. Your vet may manage bacterial or fungal infections, adjust nutrition, and monitor hydration and weight. Keep the environment low-stress and follow a strict hygiene routine, because recurring infections often drive declines more than feather changes alone.
What Bird Has White Spots on Wings? ID and Health Checks
Identify birds with white wing spots and tell normal plumage from mites, feather damage, or illness with step-by-step ch


